Search the internet for “wisdom teeth aftermath video,” and you’ll have over 1.5 million options to choose from. Filming family members and friends recovering from dental anesthesia has become a huge social media trend. Several hilarious examples – including this one and this one shown above – have gone viral, generating hundreds of millions of views and national TV coverage.
What Are They?
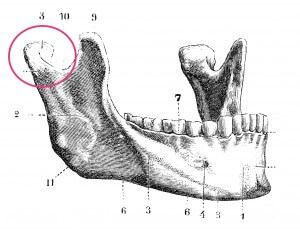
Wisdom teeth – also called 3rd molars – are the only teeth that don’t develop until after we’re born. Most often they start to emerge in late adolescence, usually between ages 17-24. Humans have always had wisdom teeth, but have become a problem our modern diets are short in specific key nutrients that are critical to bone and jaw development. Because of that, the 3rd molars crowd the rest of the teeth, potentially causing serious oral and other health problems. There are approximately 10 million wisdom teeth removed each year, at an estimated cost of more than $3 billion.
How Much Ouch?
Despite producing some of the internet’s funniest moments, wisdom tooth extraction is a routine medical procedure. It is usually performed under full sedation, which carries some minor risks. However, the procedure is fairly straightforward, and very few instances of serious complications occur. After tooth removal, the resulting wounds are packed with gauze. Patients are restricted to a liquid diet during recovery, which lasts 3-4 days. In some cases, medication may be prescribed to manage short-term pain.
It is extremely important to adhere to the treatment and follow-up recommendations. Failing to do so can lead to excessive swelling, discomfort, infection or a painful condition known as dry socket. Fortunately, the remedy for dry socket is simply to remain fully hydrated post-surgery, rinse your mouth frequently, and avoid drinking from a straw during your recovery
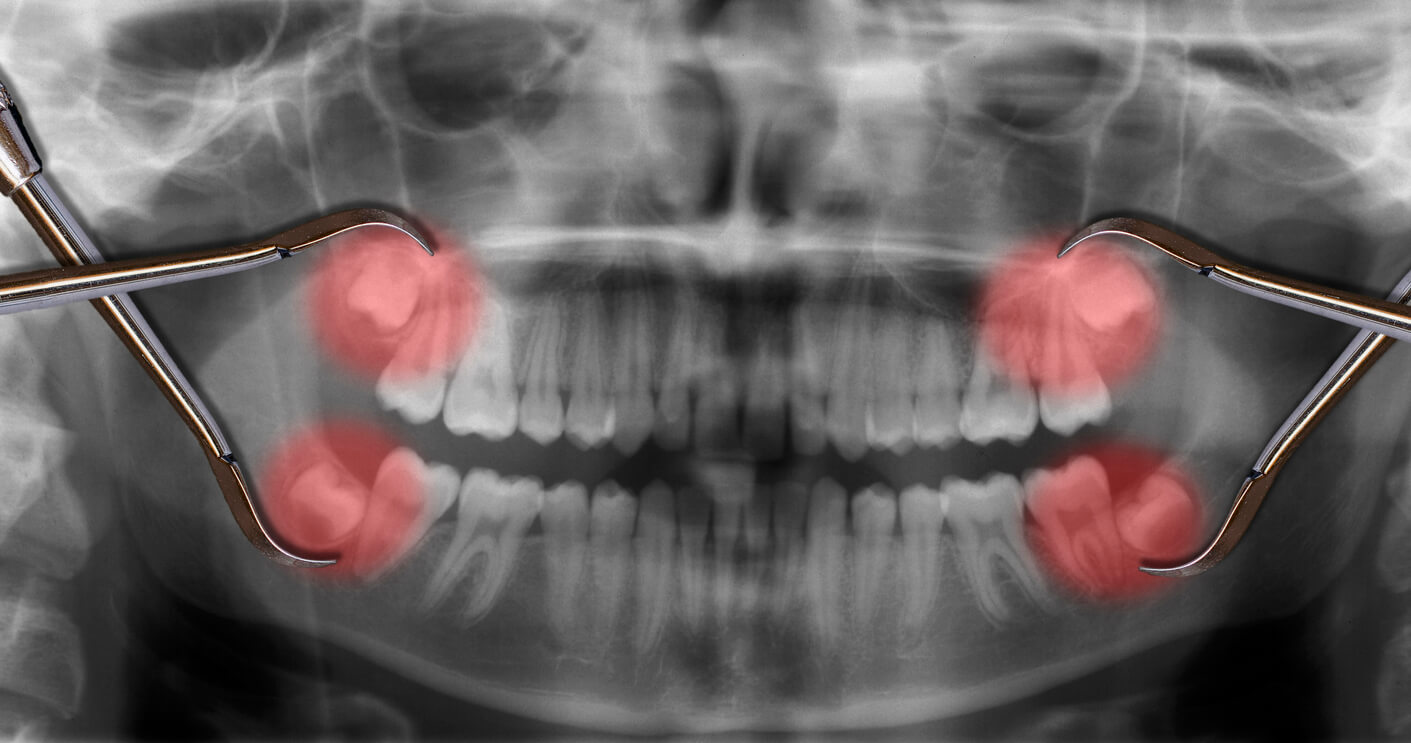
But what about MY teeth?
In past decades, it was commonplace to have 3rd molars removed as a preventative measure against potential future problems. However, since 2000 public health policy has been shifting away from the routine removal of asymptomatic wisdom teeth, according to a study published in the National Center for Biotechnology Information. However, while adopting a wait-and-see approach can avoid a potentially unnecessary procedure, both the patient and the dentist must vigilant. Regular check-ups help to monitor for signs of potential problems through roughly age 30. This follow-through is important, since complications like pericoronitis, unchecked decay, or infected roots can create serious health issues.
The bottom line is to always maintain good communication with your dentist through regular checkups, exams and X-rays. Drs. Meyer and Johns will explain how your 3rd molars are developing, and what problems you may expect from your teeth.
Have more questions? Ask us at your next appointment.